By Beth Gilbert HealthDay Reporter
The annual meeting of the American Academy of Otolaryngology-Head and Neck Surgery was held from Sept. 28 to Oct. 1 in Miami, drawing participants from around the world, including otolaryngologists, medical experts, allied health professionals, and administrators. The conference highlighted the latest advances in the diagnosis and treatment of disorders of the ears, nose, throat, and related structures of the head and neck.
In one study, Jayant Pinto, M.D., of the University of Chicago, and colleagues found that long-term exposure to environmental pollutants increases the risk for head and neck cancers (HNCs), and this risk is further elevated among those with genetic susceptibility.
The aim of the study was to evaluate the interaction between genetic and environmental determinants of HNC. As part of the National Institutes of Health All of Us research program, particulate matter ≤2.5 μm (PM2.5) air pollution exposure among adults was determined using validated spatiotemporal models. The authors used logistic regression to test the relationship between the PM2.5 level and HNC. They also performed genome-wide association studies among 906 adults with HNC and 4,310 healthy controls to identify HNC-associated single-nucleotide polymorphisms (SNPs) and gain insight into the role of these SNPs in the PM2.5 exposure-HNC relationship. An interaction between higher air pollution exposure and individuals with a genetic predisposition to developing HNC was observed. The researchers believe that interplay between these genes and pollution will help provide insight into oncogenic and targeted pathways.
“This work establishes that environmental exposures in the airway can interact with genetic susceptibility to affect the development of HNC. We need to consider these exposures when looking at cancer mechanisms and try to target pathways involved,” Pinto said. “Clinicians should be aware of these detrimental effects and encourage their patients to reduce their exposures to air pollution. We’ve done this for smoking!”
In a retrospective cohort study, Colin T. Huntley, M.D., of the Thomas Jefferson University Hospital in Philadelphia, and colleagues found that a modified sleep apnea scoring system (mSASI) may offer additional benefits in assessing obstructive sleep apnea risk severity based on cardiovascular risk factors compared with the standard apnea hypopnea index (AHI).
The AHI is the standard assessment of obstructive sleep apnea severity, but the AHI is only a single metric and does not provide a holistic assessment of the individual patient’s disease severity. As such, the authors evaluated the mSASI, which incorporates patient anatomy, symptoms, and physiologic variables to create a composite disease severity score. They hypothesized that this scoring system would be a better predictor of cardiovascular risk. The researchers found that a higher mSASI score, which represents more severe disease, was associated with a higher Framingham risk score and, therefore, supported their hypothesis. Meanwhile, the AHI was not found to be associated with an increased Framingham score.
“The AHI is a good metric but may not be the best tool to assess overall disease severity given the complexity of obstructive sleep apnea, the impact on patient quality of life, and the risk of downstream cardiovascular disease,” Huntley said. “Obstructive sleep apnea is a complex disease and the apnea hypopnea index is the current metric used to assess disease severity. With further research, new assessment tools may be available which provide a more holistic assessment of the individual patient’s disease.”
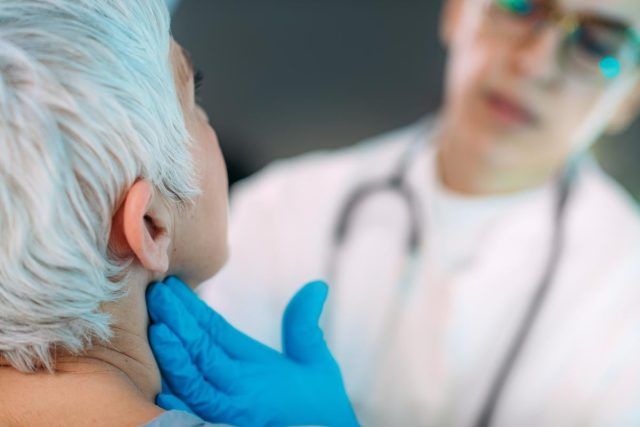
In a prospective study, Garth Olson, M.D., of the University of New Mexico in Albuquerque, and colleagues found that a standardized counseling approach regarding pain management tied to endocrine surgery is associated with reduced opioid prescriptions.
The authors developed and implemented a standardized perioperative pain management routine following endocrine surgery that involved the use of ibuprofen and counseling regarding pain. Eighty patients for whom the standardized perioperative pain management routine was implemented were followed and compared to 160 patients who had endocrine surgery without the pain management routine. The researchers found that the standardized counseling approach reduced opioid prescriptions by 46.6 percent.
“Standardized counseling about pain, including expectations and adjunctive measures, reduces opioid prescriptions in patients undergoing routine endocrine surgery,” the authors write. “Further study is needed to better understand which patients require opioid prescriptions and how perioperative pain counseling alters patient experiences with postoperative pain.”
Copyright © 2024 HealthDay. All rights reserved.